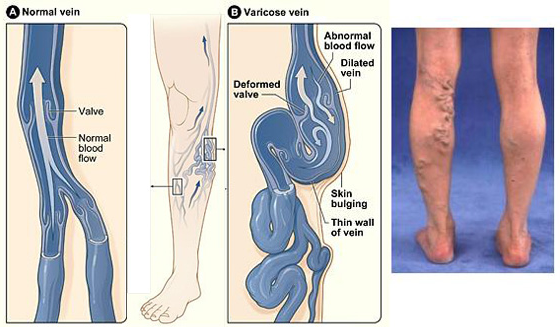
Figure A shows a normal vein with a properly working valve. In Figure B, the varicose vein has a faulty valve, the walls of the vein are thin and stretched.
More than 15 to 20 percent of all adults i.e. 1 in 5 adults in the India are affected by varicose veins. Varicose veins are enlarged, swollen, and twisting veins, often appearing blue or dark purple. They happen when faulty valves in the veins allow blood to flow in the wrong direction or to pool.
The veins have one-way valves so that the blood can travel in only one direction. If the walls of the vein become stretched and less flexible (elastic), the valves may get weaker. A weakened valve can allow blood to leak backward and eventually flow in the opposite direction. When this occurs, blood can accumulate in the vein(s), which then become enlarged and swollen.
The veins furthest from the heart are most often affected, such as those in the legs. This is because gravity makes it harder for blood to flow back to the heart. Any condition that puts pressure on the abdomen has the potential to cause varicose veins; for instance, pregnancy, constipation and, in rare cases, tumors.
Symptoms of Varicose Veins
In most cases, there is no pain, but signs and symptoms of varicose veins may include: veins look twisted, swollen, and lumpy (bulging) and the veins are blue or dark purple
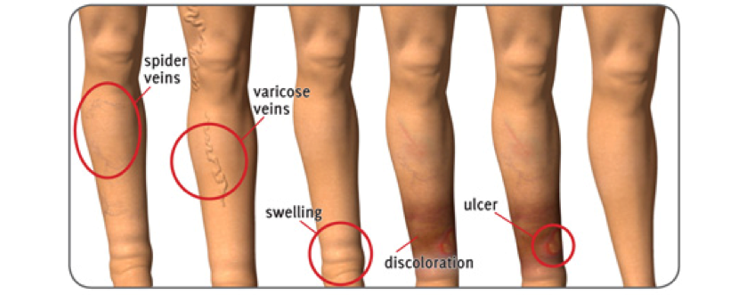
Some patients may also experience:
- Aching legs – legs feel heavy, especially after exercise or at night
- Abnormal bleeding – a minor injury to the affected area may result in longer bleeding than normal
- Swelling – swollen ankles
- Spider veins – telangiectasia in the affected leg
- Skin Discoloration – there may be a shiny skin discoloration near the varicose veins, usually brownish or blue in color
- Venous eczema – skin in the affected area is red, dry, and itchy
- Leg cramps: when suddenly standing up, some individuals experience leg cramps
- A high percentage of people with varicose veins also have restless legs syndrome
- Atrophie blanche – irregular whitish patches that look like scars appear at the ankles
Complications of Varicose Veins
Any condition in which proper blood flow is undermined has a risk of complications. However, in most cases, varicose veins have no complications. If complications do occur, they may include:
- Thrombophlebitis: Blood clots in the vein of the leg cause inflammation of the vein.
- Chronic venous insufficiency – the skin does not exchange oxygen, nutrients, and waste products with the blood properly because the blood flow is weak. Chronic venous insufficiency is not caused by varicose veins, but the two entities are closely related.
People with chronic venous insufficiency may develop varicose eczema, lipodermatosclerosis (hard and tight skin), and venous ulcers. Venous ulcers classically form around ankles and are often preceded by a discolored area. It is important to get medical evaluation for chronic venous insufficiency.
Risk Factors of Varicose Veins
Experts are not sure why the walls of veins stretch or why the valves become faulty. In many cases, it occurs for no clear reason. The following risk factors are linked to a higher risk of having varicose veins:
- Gender:Varicose veins affect women more often than males. It may be that female hormones relax veins. If so, taking birth control pills or hormone therapy (HT) might contribute.
- Genetics:Varicose veins often run in families.</li >
- Obesity:Being overweight or obese increases the risk of varicose veins.
- Age:The risk increases with age, due to wear and tear on vein valves.
- Some jobs:An individual who spend a long time standing at work may have a higher chance of varicose veins.
Treatment for Varicose Veins
If the patient has no symptoms or discomfort and is not bothered by the sight of the varicose veins, treatment might not be necessary. However, if there are symptoms, treatment may be required to reduce pain or discomfort, address complications, such as leg ulcers, skin discoloration, or swelling.
Some patients may also want treatment for cosmetic reasons – they want to get rid of the “ugly” varicose veins.
In severe cases, a varicose vein may rupture, or develop into varicose ulcers on the skin. These will require treatment.
- Surgery
If varicose veins are large, they may need to be removed surgically. This is usually done under general anesthetic. In most cases, the patient can go home the same day – if surgery is required on both legs, they may need to spend one night in hospital.
- Ligation And Stripping
Two incisions are made, one near the patient’s groin at the top of the target vein, and the other is made further down the leg, either at the ankle or knee. The top of the vein is tied up and sealed. A thin, flexible wire is threaded through the bottom of the vein and then pulled out, taking the vein with it.
This procedure does not usually require a hospital stay. Ligation and stripping can sometimes result in bruising, bleeding, and pain. In extremely rare occasions, there may be deep vein thrombosis.
After surgery, most patients will need 1-3 weeks to recover before going back to work and other normal duties. During recovery time, compression stockings are worn.
- Sclerotherapy
A chemical is injected into small and medium-sized varicose veins, which scars and closes them. A few weeks later, they should fade. A vein may need to be injected more than once.
- Radiofrequency Ablation
A small incision is made either above or below the knee, and with the help of an ultrasound scan; a narrow tube (catheter) is threaded into the vein.
The doctor inserts a probe into the catheter, which emits radiofrequency energy. The radiofrequency energy heats up the vein, causing its walls to collapse, effectively closing it and sealing it shut. This procedure is preferred for larger varicose veins. Radiofrequency ablation is usually done with a local anesthetic.
- Endovenous Laser Ablation (EVLA)
A catheter is inserted into the patient’s vein. A small laser is threaded through the catheter and positioned at the top of the target vein; it delivers short energy bursts that heat up the vein, sealing it shut.
With the aid of an ultrasound scan, the doctor threads the laser all the way up the vein, gradually burning and sealing all of it. This procedure is done under local anesthetic.
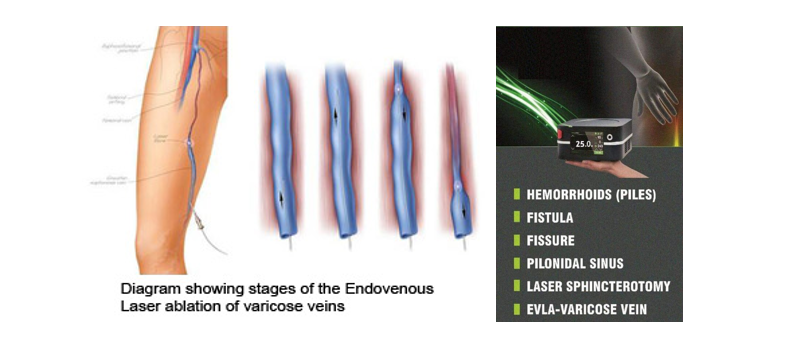
Post-EVLA Instructions:
- Compression stockings will be in place initially.
- Normal activities can be resumed immediately.
- Exercise programs can be resumed after two weeks.
- There is no incision, no stitches, no scars…and no veins.
6. Transilluminated Powered Phlebectomy
An endoscopic transilluminator (special light) is threaded through an incision under the skin so that the doctor can see which veins need to be taken out. The target veins are cut and removed with a suction device through the incision.
A general or local anesthetic may be used for this procedure. There may be some bleeding and bruising after the operation.
Pregnancy And Varicose Veins
Women are much more likely to develop varicose veins during their pregnancy than at any other time in their lives. Pregnant women have much more blood in their body; this places extra pressure on the circulatory system.
Additionally, changes in hormone levels can lead to a relaxation of the blood vessel walls. Both these factors raise the risk of having varicose veins.
As the uterus (womb) grows, there is more pressure on the veins in the mother’s pelvic area. In the majority of cases, the varicose veins go away after the pregnancy is over; this is not always the case, and sometimes, even if the varicose veins improve, there may be some left visible.
Preventing Measures
Getting plenty of exercise is the best way to ward off spider veins and varicose veins. Exercise helps keep your weight under control and your leg muscles toned, so your blood will flow freely.
If your job keeps you on your feet, stretch your leg muscles often to increase circulation.And if you’re pregnant, try to sleep on your left side rather than your back.

